In 2004 a multidisciplinary team of researchers from Penn State University lead by Carol Weisman, PhD, Distinguished Professor of Public Health Sciences, Obstetrics and Gynecology, and Health Policy and Administration and Associate Dean for Faculty Affairs, College of Medicine, and working in collaboration with colleagues from Franklin and Marshall College, Lock Haven University, and the Family Health Council of Central Pennsylvania were awarded a $4.7 million grant from the Pennsylvania Department of Health to embark on the four-year Central Pennsylvania Women’s Health Study (CePAWHS). The project’s goal was to reduce adverse pregnancy outcomes by improving women’s health prior to pregnancy in central Pennsylvania. As a first step, 2,002 women in the general population and 288 Amish women residing in 28 counties in Central PA were interviewed about their health status and risks. Using what they learned from these interviews, the investigators developed the Strong Healthy Women (SHW) intervention.
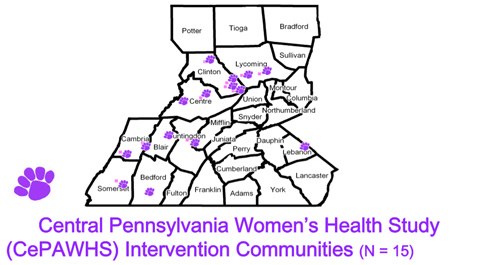
Grounded in the social cognitive approach to behavior change, SHW was aimed at improving the health of women who had not yet become pregnant or who were between pregnancies. Specifically, the intervention targeted: poor nutrition, low physical activity, tobacco and alcohol use and exposure, unhealthy strategies for coping with stress, gynecologic infections, and inadequate pregnancy planning or spacing. The SHW study participants were 692 women living in 15 low-income rural communities, who were randomly assigned to the intervention or a control group. Those assigned to the intervention condition attended 6 small group sessions conducted over a 12-week period.
Improving women’s health before they become pregnant is a potent strategy for reducing adverse pregnancy outcomes, as recommended by the Centers for Disease Control and Prevention. Further, an emphasis on pre-pregnancy health has garnered attention because waiting until a woman is pregnant may be too late to reduce the health risks in early pregnancy and may be the best chance of attaining good outcomes for both mothers and infants.
Information on their health and health behaviors was collected 14 weeks after participants completed the SHW program, and again at 6-months and 12-months post-completion. Pretest-posttest results revealed that women who received the intervention, compared to controls, had greater perceived control of birth outcomes and were more likely to: read food labels for nutritional facts, eat healthy foods, comply with recommended daily levels of physical activity, and take a daily multivitamin containing folic acid. In a new article published in the current issue of Women’s Health Issues the investigators reported data from the 12 month post intervention follow-up showing that women from the intervention group maintained their use of a daily multivitamin and also had lower weight and BMIs compared to women in the control group. Additionally, women in the intervention who gave birth to a singleton during this time period trended towards having lower pregnancy weight gain compared with controls.
SHW’s principal investigator, Dr. Carol Weisman, notes, “We are currently working with researchers across the country to implement the Strong Healthy Women curriculum in more economically and socially diverse populations, including in urban areas within Pennsylvania. Targeting women’s preconceptional health is integral in the effort to improve both mother and child health outcomes.”
In addition to Weisman, other researchers on the grant include Marianne Hillemeier, Associate Director, Population Research Institute and Associate Professor of Health Policy and Administration and Demography, College of Health and Human Development; John Botti, Professor of Obstetrics and Gynecology, College of Medicine; Danielle Symons Downs, Associate Professor of Kinesiology, College of Health and Human Development; Mark Feinberg, PhD, Senior Research Associate, Prevention Research Center for the Promotion of Human Development, College of Health and Human Development; Cynthia Chuang, Associate Professor of Medicine, College of Medicine; and Anne-Marie Dyer, MS, Biostatistician/Scientific Coordinator, Public Health Sciences, College of Medicine.